Waking up with sudden, stabbing back pain that makes it impossible to stand straight is a terrifying experience. For many, especially those dealing with osteoporosis, this is the reality of a vertebral compression fracture. When bracing and painkillers aren't enough, you're often faced with two similar-sounding options: kyphoplasty is a minimally invasive procedure that uses a balloon to restore vertebral height before injecting bone cement. On the other hand, there is vertebroplasty, which skips the balloon and goes straight to the cement. While both aim to stop the pain and stabilize the spine, they aren't identical. If you're trying to figure out which one makes sense for your situation, you need to know how they actually differ in terms of recovery, risk, and long-term results.
The Basics: How These Procedures Work
Both treatments fall under the umbrella of vertebral augmentation. They are designed for people whose vertebrae have collapsed due to osteoporosis, trauma, or cancer. The goal is simple: stabilize the bone and kill the pain.
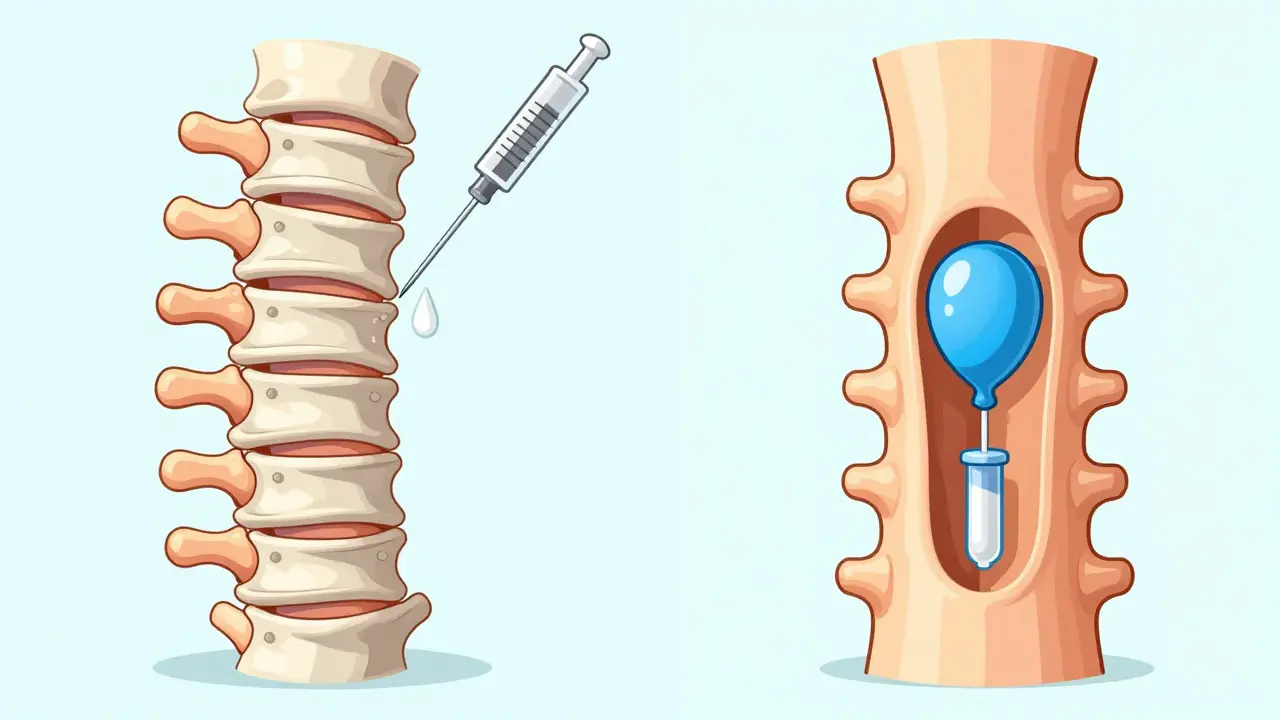
In a vertebroplasty, a doctor uses a needle to inject polymethylmethacrylate (PMMA)-a medical-grade bone cement-directly into the fractured bone. This happens under a live X-ray called fluoroscopy. The cement hardens in about 10 to 20 minutes, essentially "gluing" the fracture together. It's a fast process, usually taking 30 to 60 minutes.
Kyphoplasty adds a clever step. Before the cement goes in, the surgeon inserts a small balloon (about 8-15mm) into the collapsed bone and inflates it. This pushes the bone back up, recreating some of the original height of the vertebra. Once the space is created, the balloon is deflated and removed, and the PMMA cement is injected into the newly formed cavity. Because the balloon creates a void, the cement doesn't have to be pushed in under as much pressure.
Key Differences: Height, Pain, and Safety
If you only care about pain, the good news is that both procedures are incredibly effective. Patients typically report an 85-90% reduction in pain almost immediately. You might go from an 8 out of 10 on the pain scale to a 1 or 2 within 24 hours. However, the "structural" results are where they diverge.
Kyphoplasty is the clear winner for restoring the shape of your spine. Biomechanical studies show it can restore 40-60% of lost vertebral height. This is why it's usually the go-to for fractures with significant deformity (over 30% height loss). Vertebroplasty, by contrast, provides almost no height restoration; it simply stops the bone from collapsing further.
Safety is another major talking point. A significant risk with these procedures is "cement leakage," where the glue seeps out of the bone. Vertebroplasty has a higher leakage rate, ranging from 27% to 68%. Kyphoplasty is safer in this regard, with leakage rates between 9% and 33%. This is because the balloon in kyphoplasty creates a controlled space, meaning the cement doesn't need to be forced through the bone's pores under high pressure.
| Feature | Vertebroplasty | Kyphoplasty |
|---|---|---|
| Primary Goal | Pain relief & stability | Pain relief, stability & height restoration |
| Procedure Method | Direct cement injection | Balloon inflation then cement injection |
| Height Restoration | Minimal | Significant (40-60%) |
| Cement Leakage Risk | Higher (27-68%) | Lower (9-33%) |
| Average Cost (Medicare) | Approx. $2,950 | Approx. $3,850 |
Which One Should You Choose?
The decision usually comes down to the severity of the collapse and your specific health needs. If your fracture is stable and you just want the pain to stop, vertebroplasty is a high-value, efficient option. It's cheaper and faster, and the pain relief is virtually identical to its counterpart.
However, if you are dealing with a significant "hunch" or kyphotic deformity, kyphoplasty is the better bet. Restoring height can help with posture and potentially reduce the pressure on adjacent vertebrae. It's also generally preferred for patients with very poor bone quality, as the lower-pressure injection reduces the risk of cement traveling to other parts of the body.
It is worth noting that the height gains from kyphoplasty aren't always permanent. Some data suggests that over time and through thousands of loading cycles (just walking and moving), that restored height can drop by about 30%. You aren't necessarily getting your 20-year-old spine back, but you are getting a more stable foundation.
Recovery and What to Expect After Surgery
One of the best parts of these procedures is that they aren't like traditional open-back surgery. You aren't looking at weeks of bed rest. Most patients go home the same day. In fact, about 92% of people return to their normal activities within just 72 hours. For many, the most immediate benefit is a reduced reliance on heavy painkillers; roughly 75% of patients stop using opioids within a week after the procedure.
The immediate post-op window requires a little caution. You'll usually have a 4-to-6 hour monitoring period and some weight-bearing restrictions for the first 24 hours. After that, you'll gradually ramp up your activity over one to two weeks. The most common "downside" reported by patients isn't the surgery itself, but the rare occurrence of a new fracture in a neighboring vertebra, which happens in about 5-10% of cases within the first year. This is often due to the underlying osteoporosis rather than the procedure itself.

The Role of Modern Imaging and Tech
You can't just walk in and get these done. Doctors require a recent MRI-usually within the last six weeks-to confirm that the fracture is "acute." This means they look for bone marrow edema (swelling). If a fracture is old and the inflammation is gone, these procedures won't help much and are generally contraindicated.
Technology is also evolving. We are seeing the rise of calcium phosphate cements. Unlike the standard PMMA, these better mimic real bone and don't generate as much heat during the hardening process, which reduces the risk of thermal damage to surrounding tissues. Additionally, newer balloon systems are making the kyphoplasty process even more precise, which is why it's slowly becoming the dominant choice in the US market.
Is kyphoplasty more painful than vertebroplasty?
Not necessarily. Both procedures use local anesthesia and intravenous sedation or general anesthesia, meaning you won't feel the procedure. The recovery time and immediate pain relief levels are very similar for both.
How long does the bone cement last?
The PMMA cement is designed to be permanent. It creates a stable, hardened column within the vertebra that provides long-term support and pain relief. While the height restored by a balloon may diminish slightly over years, the stabilization provided by the cement remains.
Will insurance or Medicare cover these procedures?
Yes, Medicare approval rates are very high (often over 95%) provided you can document that conservative treatments failed. This usually means you've tried bracing, physical therapy, and pain medication for at least 4 to 6 weeks without success.
Can these procedures cure osteoporosis?
No. These are structural repairs for a specific fracture. They do not treat the underlying cause of osteoporosis. It is crucial to continue medical treatment for bone density to prevent future fractures in other parts of your spine.
What are the risks of cement leakage?
Cement leakage occurs when the glue escapes the vertebral body. While common, it's rarely dangerous. However, in about 0.6% to 1.1% of cases, it can lead to serious issues like pulmonary embolisms or nerve compression. Kyphoplasty generally has a lower risk of this occurring.
Next Steps for Patients
If you're currently struggling with a vertebral fracture, your first step is to get a fresh MRI to see if your fracture is still in the "acute" phase. Once confirmed, sit down with your surgeon and ask specifically about your height loss. If you've lost more than 30% of the vertebra's height or are noticing a significant curve in your back, push for a discussion on kyphoplasty.
For those who are more concerned about cost or have a very stable fracture, vertebroplasty is an excellent, efficient path to pain relief. Regardless of the choice, ensure you have a post-operative plan that includes a bone density specialist to manage your osteoporosis, as the most successful spinal surgery is the one you never need because your bones stayed strong.
Joel Bonstell
Had a similar thing happen to my dad last year and it realy is as scary as it sounds. We went with the kyphoplasty because he had some height loss and it honestly changed his life. Just make sure you follow the post-op rules closely or you risk messin up the stabilization.
Robert Cowley
Typical medical propaganda 🙄 Like anyone actually believes those leakage percentages. It's all just a way to push the more expensive procedure on scared old people. Absolute joke! 🤡
Sarah Mifsud
Great breakdown. One thing to add is that physical thera py after the initial healing phase is a huge deal. It helps get the core muscles back so the neighboring vertebrae dont take all the stress.
Ken Baldridge
The mention of bone marrow edema is key here. If you're seeing a clinician who isn't checking for that acute inflammatory phase via MRI, they're basically guessing. Proper diagnostic triage is the only way to ensure the PMMA actually addresses the symptomatic site without causing secondary complications.
Christina Lancey
It is so encouraging to see that the recovery time is relatively short. For anyone feeling overwhelmed, just take it one day at a time.
Rebekah Korak
It's fascinating, really, how we obsess over the structural architecture of the spine as if the physical body is the only thing that defines our stability in this chaotic existence. We treat the vertebra like a crumbling building, injecting cement to stave off the inevitable decay of time, yet we forget that the alignment of the soul is far more critical than whether one has lost thirty percent of their height. People just blindly follow these medical guidelines without questioning the existential cost of becoming a cyborg of PMMA and balloons, thinking a few millimeters of height will somehow return them to a youth that is long gone and frankly, irrelevant to the current state of their consciousness. It's a classic case of focusing on the symptom rather than the spiritual void that often accompanies the aging process.
SWATI NAWANGE
The sheer simplicity of the comparison table is almost insulting to those of us who understand the nuances of spinal biomechanics. It is quite pedestrian to suggest that cost is a primary driver when the clinical outcome is so clearly superior with kyphoplasty.
Kartik Agarwal
I would suggest looking into the synergistic effects of combining these procedures with pharmacological interventions to improve BMD. The goal is to mitigate the risk of adjacent segment fractures through comprehensive metabolic management.
nikki paurillo
The spine is like a weathered old tree, sometimes we just need a little structural support to keep our spirit reaching for the sky. This is a lovely way to explain the alchemy of modern medicine blending with the frailty of our human frames.
Bradley Gusick
You see how they push the 'new' cements? Probably just another way for the government to track our bone density from the inside. They want us stabilized and predictable. Wake up! The medical industry is just a front for total biological control!
Leah Sentz
Exactly!! 🇺🇸 My uncle had this and the doctors were total hacks! 😡 I can't even deal with how some people just accept this garbage! 😱😭💔
Tallulah Sandison
Just do it! 🚀 Fast recovery is the best part. Dont let the fear stop u!